If you’ve ever spent weeks diligently “squeezing and lifting” only to feel absolutely no change in your body, you aren’t alone. For many women—especially those navigating postpartum recovery or noticing a dip in sensation over time—the traditional manual Kegel feels like throwing a pebble into a dark well. You hope it’s doing something, but you never hear the splash.
The truth is that pelvic floor recovery isn’t just about strength; it’s about neurological connection and blood flow. When you lose that “tighter” feeling or struggle to reach peak arousal, your body is telling you that the communication line between your brain and your pelvic floor is frayed. To fix it, we need to move beyond 1940s-era exercises and embrace a modern, tech-assisted approach to sensitivity restoration.
The Limitation of “Blind” Kegels: Why You’re Not Seeing Results
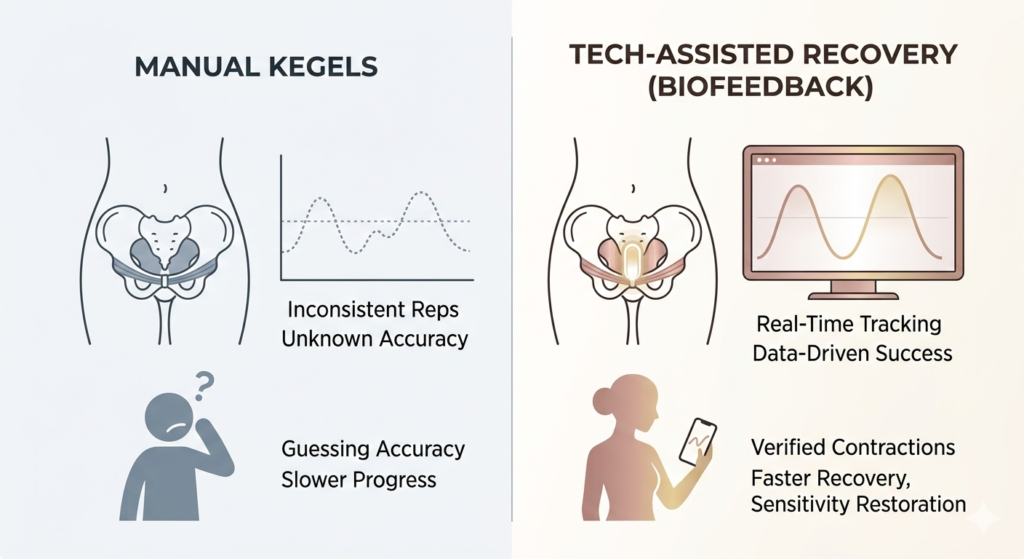
The biggest hurdle in pelvic floor recovery is isolation. Unlike your biceps, you can’t see your pelvic muscles in a mirror. Research shows that nearly half of women attempting manual Kegels are either using the wrong muscles (like their abs or glutes) or, worse, pushing downward—which can actually exacerbate issues like prolapse or leaks.
Without biofeedback, you are essentially training in the dark. If you can’t measure the contraction, you can’t improve the tone. This “blind” training is the primary reason why many give up before they see any real-world improvement in their intimate life.
The Science of Sensitivity: How Muscle Tone Dictates Pleasure
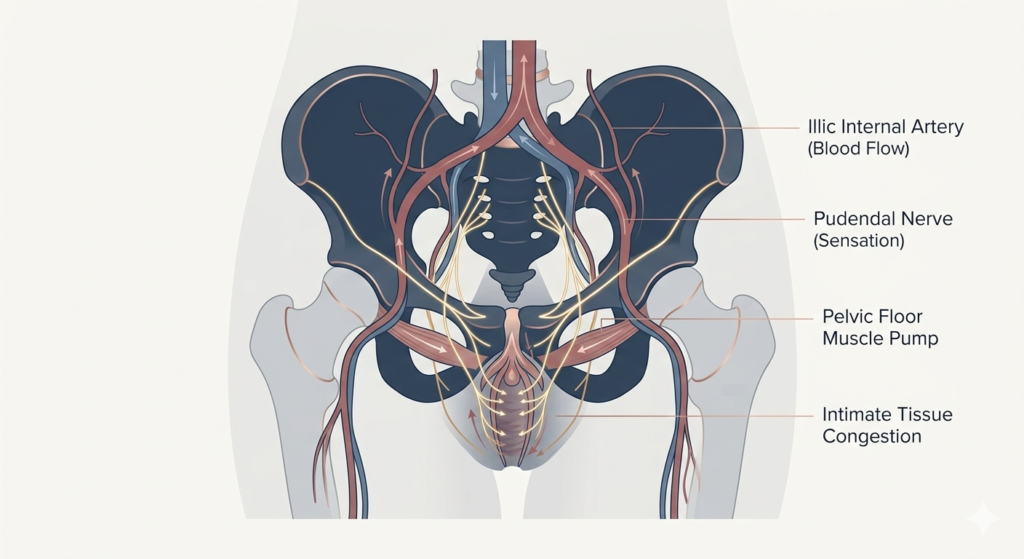
We often think of muscles only in terms of strength, but in the pelvic region, muscles serve a second, critical purpose: they act as a biological pump.
Every time your pelvic floor contracts and relaxes, it flushes the area with fresh, oxygenated blood. This isn’t just about health; it’s about sensitivity restoration. Chronic “numbness” or a lack of response is often caused by poor micro-circulation. When your muscles are toned and active, they sustain the engorgement necessary for heightened sensation. A strong pelvic floor literally paves the neural highways that allow for more intense, frequent peaks.
Modern Recovery Strategy 1: Smart Biofeedback Devices
The most significant leap in intimate wellness has been the miniaturization of biofeedback technology. Modern smart trainers, like those curated by PureInti, act as a “personal trainer” for your inner core.
These devices use high-precision pressure sensors to tell you exactly when you are hitting the right muscle. By connecting to an app, they turn a boring chore into a data-driven workout. You can see your grip strength, track your endurance over weeks, and ensure that every minute you spend training is actually moving the needle toward recovery.
Modern Recovery Strategy 2: Vibration Therapy for Nerve Re-Education
Sometimes, the connection is so dampened that you can’t even “find” the muscle to squeeze it. This is common after childbirth or long periods of inactivity. This is where vibration therapy becomes a therapeutic tool.
Specific medical-grade frequencies can trigger “involuntary” contractions. This “wakes up” the nerves and forces the muscles to react, even if your brain-to-muscle connection is currently weak. According to the Mayo Clinic, consistent stimulation of these nerves is key to treating stress incontinence and Improving the physiological response to intimacy.
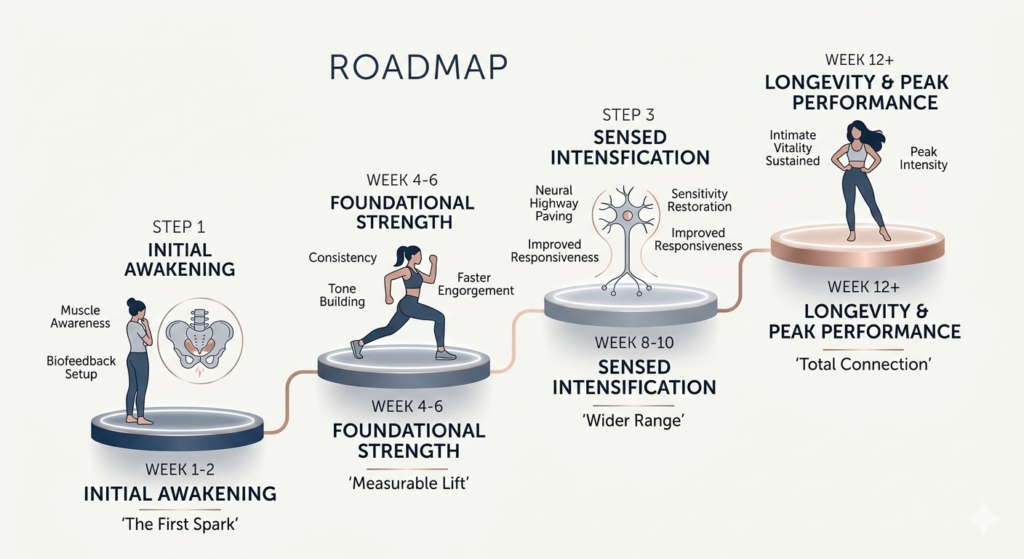
Creating Your 12-Week Roadmap to Restoration
Recovery doesn’t happen overnight, but with the right tech, it happens much faster than manual methods. Here is how a structured pelvic floor recovery plan looks:
| Phase | Timeline | Focus | The Result |
| Phase 1 | Week 1-4 | Neural Activation | “Waking up” the nerves; stopping the “blind” squeezing. |
| Phase 2 | Week 5-8 | Strength & Hypertrophy | Measurable increase in grip and lift strength. |
| Phase 3 | Week 9-12 | Sensitivity Peak | Noticeable improvement in natural lubrication and response. |
FAQ: Solving the Modern Recovery Puzzle
Q: Can I use these devices if I have an IUD? A: Generally, yes. Most medical-grade silicone devices are perfectly safe with an IUD, but we always recommend a quick chat with your OB-GYN to ensure your specific placement is clear.
Q: How soon after giving birth can I start? A: The “Golden Window” usually starts after your 6-week postpartum checkup. Once your doctor clears you for internal activity, tech-assisted recovery can significantly speed up the healing of the vaginal canal and pelvic base.
Q: Is “over-training” a thing? A: Yes. Like any muscle, the pelvic floor can become “hypertonic” (too tight) if you don’t practice relaxation. Modern smart devices are great because they teach you to relax the muscle just as much as they teach you to squeeze it.
Your Next Step for Intimate Wellness
Reclaiming your body shouldn’t be a guessing game. By moving beyond basic exercises and using data-driven tools, you can shorten your recovery time and rediscover sensations you thought were gone.
